Pre-Cancerous Lesion Treatment to Stop Skin Cancer Before It Starts
Pre-cancerous lesions are abnormal skin growths that haven’t yet become cancer but have the potential to develop into skin cancer if left untreated. Identifying and treating these lesions early is one of the most effective ways to prevent skin cancer before it starts. At Glo Dermatology in Parma, Ohio, Dr. Shaza Daoud provides expert diagnosis and treatment of pre-cancerous lesions, helping patients throughout Greater Cleveland protect their skin health and reduce their cancer risk.
If you’ve been told you have a pre-cancerous lesion or have noticed rough, scaly patches developing on sun-exposed areas of your skin, prompt evaluation and treatment are essential. Dr. Daoud offers multiple effective treatment options that can eliminate pre-cancerous cells before they progress to invasive cancer. With her expertise and personalized approach to care, you can address these concerning growths and take proactive steps to safeguard your long-term skin health.
Understanding Pre-Cancerous Lesions
Pre-cancerous lesions, also called precancers or premalignant lesions, are areas of abnormal cell growth that show signs of progressing toward cancer but haven’t yet invaded surrounding tissues. Think of them as an early warning system—your skin is telling you that damage has occurred and that without intervention, cancer could develop.
The most common type of pre-cancerous skin lesion is actinic keratosis, but other conditions can also be considered precancerous. What these lesions share in common is that they represent an opportunity for prevention. By treating pre-cancerous lesions before they become cancer, you can avoid the more extensive treatments and potential complications associated with skin cancer.
Not every pre-cancerous lesion will progress to cancer, but there’s no reliable way to predict which ones will and which won’t. Because the treatments for pre-cancerous lesions are generally simpler, less invasive, and more effective than treatments for established skin cancer, the standard of care is to treat these lesions when they’re identified.
Actinic Keratosis: The Most Common Pre-Cancerous Lesion
Actinic keratosis (AK), also called solar keratosis, is the most frequently diagnosed pre-cancerous skin condition. These lesions develop from years of cumulative sun exposure and are extremely common—an estimated 58 million Americans have one or more actinic keratoses.
What Actinic Keratosis Looks Like
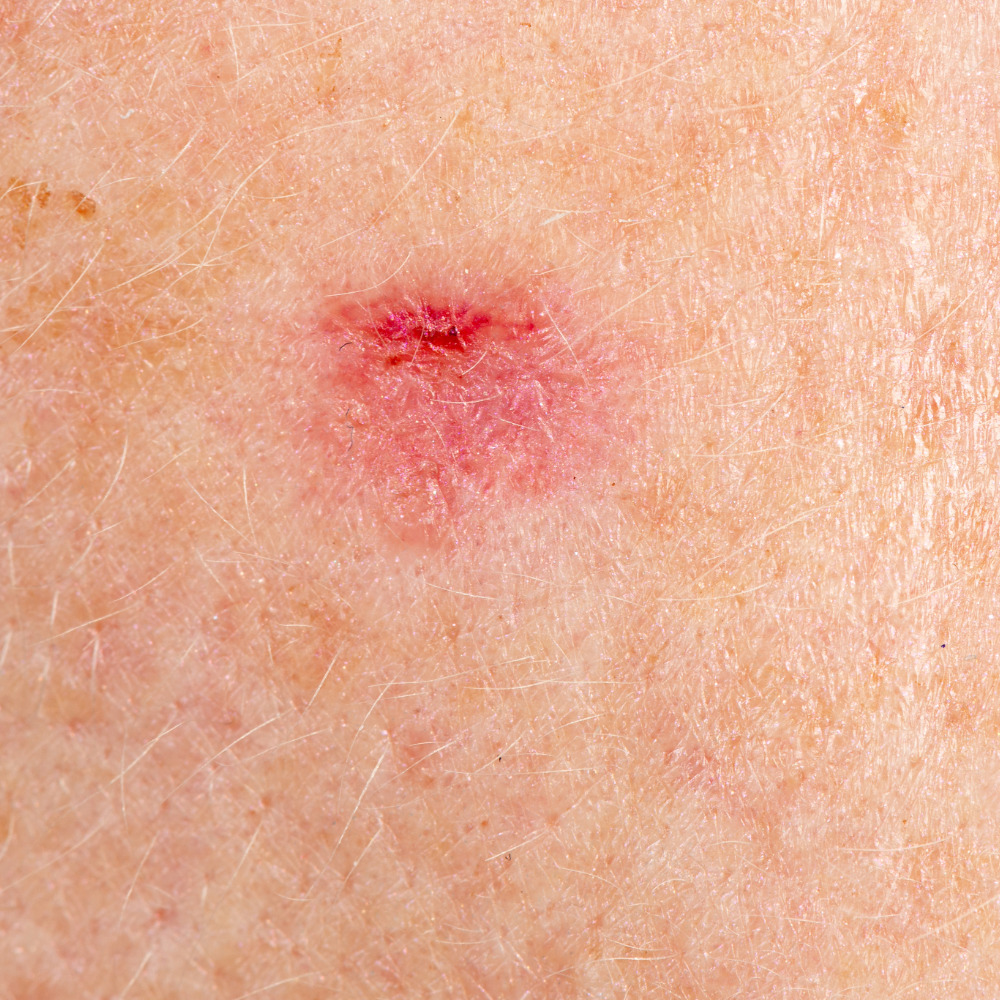
Actinic keratoses typically appear as rough, dry, scaly patches or spots on the skin. They range in size from a small spot to an inch or more in diameter. The texture is often described as feeling like sandpaper—you may feel an AK before you can see it. Color varies from skin-toned to pink, red, tan, or brown. Some AKs have a hard, wart-like surface, while others are flat.
These lesions most commonly develop on areas of the body that receive the most sun exposure over time, including the face (especially the forehead, nose, cheeks, and lips), ears, scalp (particularly in people with thinning hair or baldness), neck, backs of the hands, forearms, and lower legs (especially in women).
Actinic keratoses may come and go—sometimes they seem to disappear on their own, only to return weeks or months later. They may itch, burn, or feel tender. Some AKs become inflamed, red, and more noticeable, while others remain subtle.
The Risk of Progression
While most actinic keratoses don’t progress to cancer, an estimated 5 to 10 percent will develop into squamous cell carcinoma if left untreated. Because there’s no way to determine which AKs will become cancerous, dermatologists recommend treating all actinic keratoses.
Signs that an actinic keratosis may be progressing include rapid growth, increasing thickness or elevation, hardening of the lesion, bleeding or ulceration, pain or tenderness, and development of a horn-like projection.
If you notice any of these changes in an existing AK or any other skin lesion, contact Glo Dermatology promptly for evaluation.
Other Pre-Cancerous Skin Conditions
While actinic keratosis is the most common pre-cancerous lesion, other conditions also warrant attention and treatment.
Actinic Cheilitis
Actinic cheilitis is essentially actinic keratosis of the lips, most commonly affecting the lower lip. It causes persistent dryness, cracking, and scaling of the lip, often with blurring of the border between the lip and surrounding skin. The lip may feel rough or sandpapery. Actinic cheilitis can progress to squamous cell carcinoma and should be treated when identified.
Bowen’s Disease (Squamous Cell Carcinoma In Situ)
Bowen’s disease represents squamous cell carcinoma that is confined to the epidermis (the outermost layer of skin) and hasn’t yet invaded deeper tissues. It appears as a persistent, slow-growing, red, scaly patch. While technically an early cancer rather than a pre-cancer, Bowen’s disease is highly treatable when caught at this stage, before invasion occurs.
Leukoplakia
Leukoplakia refers to white patches that develop on the mucous membranes of the mouth, tongue, or gums. While not all leukoplakia is pre-cancerous, some cases can progress to oral cancer. Leukoplakia is often associated with tobacco use and should be evaluated by a healthcare provider.
Atypical Moles (Dysplastic Nevi)
While most moles are benign, atypical moles have unusual features and are associated with an increased risk of melanoma. People with multiple atypical moles or atypical mole syndrome require regular monitoring and may need some moles removed as a preventive measure.
Risk Factors for Pre-Cancerous Lesions
Understanding your risk factors helps you take appropriate preventive measures and recognize when you should be screened for pre-cancerous lesions.
Sun Exposure
Cumulative sun exposure over your lifetime is the primary risk factor for developing actinic keratoses and other pre-cancerous lesions. This includes both intense, intermittent exposure (like beach vacations) and chronic, everyday exposure (like walking to your car, gardening, or working outdoors). The damage from UV radiation accumulates over decades, which is why pre-cancerous lesions become more common as we age.
Fair Skin
People with fair skin, light-colored eyes, and blonde or red hair are at significantly higher risk because they have less melanin to protect against UV damage. However, people with darker skin tones can also develop pre-cancerous lesions and skin cancer, particularly on sun-exposed areas.
Age
Pre-cancerous lesions become increasingly common with age due to accumulated sun damage. While they’re most common in people over 40, younger individuals with significant sun exposure can develop them too.
Geographic Location
Living in sunny climates or at high altitudes increases UV exposure and pre-cancerous lesion risk. People who live in the southern United States, for example, tend to have higher rates of actinic keratoses than those in northern states.
History of Sunburns
A history of severe sunburns, especially blistering sunburns in childhood or adolescence, significantly increases the risk of developing pre-cancerous lesions and skin cancer later in life.
Tanning Bed Use
Indoor tanning dramatically increases UV exposure and the risk of pre-cancerous lesions and skin cancer. Even occasional use of tanning beds raises risk significantly.
Weakened Immune System
People with weakened immune systems—whether due to organ transplant, HIV/AIDS, cancer treatment, or immunosuppressive medications—are at much higher risk of developing pre-cancerous lesions and having them progress to cancer.
Diagnosing Pre-Cancerous Lesions
Dr. Daoud can often diagnose actinic keratoses and other pre-cancerous lesions through visual examination. The characteristic appearance and texture of these lesions, combined with their location on sun-exposed skin, usually makes diagnosis straightforward.
During your appointment, Dr. Daoud will examine the lesions in question and may use dermoscopy—a specialized magnifying device—to evaluate them more closely. She’ll also examine the surrounding skin, as people with one actinic keratosis often have others, and sun-damaged skin is at risk for developing additional lesions over time.
In some cases, a biopsy may be recommended. This involves removing all or part of the lesion and examining it under a microscope. A biopsy is particularly important if there’s any concern that a lesion might have already progressed to skin cancer, if the diagnosis is uncertain, or if the lesion hasn’t responded to treatment as expected.
Treatment Options for Pre-Cancerous Lesions
Glo Dermatology offers multiple effective treatments for pre-cancerous lesions. The best approach depends on factors including the number, size, and location of your lesions, your overall health, your treatment preferences, and whether you’ve had pre-cancerous lesions treated before.
Cryotherapy (Freezing)
Cryotherapy is the most common treatment for individual actinic keratoses. During this quick, in-office procedure, Dr. Daoud applies liquid nitrogen to the lesion using a spray device or cotton-tipped applicator. The extreme cold destroys the abnormal cells, and the treated area typically blisters and peels off over the following days to weeks, revealing healthy skin beneath.
Cryotherapy is fast, effective, and doesn’t require anesthesia. It works well for individual lesions or small numbers of AKs. Treated areas may be temporarily lighter than surrounding skin, and there’s a small risk of scarring.
Topical Medications
For patients with multiple actinic keratoses or widespread sun damage, topical medications that treat larger areas of skin may be more practical than treating each lesion individually. Several prescription creams and gels are available.
Fluorouracil (5-FU) is a chemotherapy cream that destroys abnormal cells while sparing healthy tissue. It’s applied daily for several weeks and causes redness, crusting, and discomfort during treatment, but these effects indicate the medication is working. Once treatment is complete, the skin heals and appears healthier.
Imiquimod is an immune-modulating cream that stimulates your body’s own immune system to attack abnormal cells. Like fluorouracil, it causes a skin reaction during treatment that resolves once treatment ends.
Ingenol mebutate and diclofenac are other topical options that may be appropriate for certain patients.
Topical treatments have the advantage of treating visible lesions and subclinical (not yet visible) damage simultaneously, potentially preventing future lesions from developing.
Photodynamic Therapy (PDT)
Photodynamic therapy combines a light-sensitizing medication with specific wavelengths of light to destroy pre-cancerous cells. During PDT, a photosensitizing solution is applied to the skin and allowed to absorb for a period of time. The treated area is then exposed to a special light that activates the medication, which selectively destroys abnormal cells.
PDT is highly effective for treating multiple actinic keratoses and areas of widespread sun damage. It also has cosmetic benefits—many patients notice improved skin texture and reduced discoloration after treatment. The procedure causes temporary redness, swelling, and sensitivity that typically resolve within a week or two.
Curettage and Electrodesiccation
For thicker actinic keratoses or lesions that may have started to progress, curettage and electrodesiccation may be recommended. This procedure involves numbing the area, scraping away the abnormal tissue with a curette (a sharp, spoon-shaped instrument), and using electrical current to destroy any remaining abnormal cells and control bleeding.
Surgical Excision
In some cases, surgical removal of a pre-cancerous lesion may be recommended, particularly if there’s concern about possible progression to cancer or if a tissue sample is needed for pathological examination.
Chemical Peels and Laser Resurfacing
For patients with extensive sun damage, chemical peels or laser resurfacing can treat pre-cancerous lesions while also improving overall skin appearance. These procedures remove damaged outer layers of skin, revealing healthier skin beneath.
What to Expect After Treatment
Recovery after pre-cancerous lesion treatment varies depending on the method used.
After cryotherapy, you can expect redness, swelling, and possibly blistering at the treatment site. A scab will form and fall off over one to three weeks. Keep the area clean and protected until healed.
Topical treatments cause a predictable skin reaction during the treatment period, including redness, scaling, crusting, and discomfort. This is normal and indicates the medication is working. The skin heals after treatment ends, typically looking healthier than before.
After photodynamic therapy, expect redness, swelling, and sensitivity for several days to two weeks. Strict sun avoidance is essential immediately after PDT because the photosensitizing medication remains active in your skin.
Regardless of treatment method, protect treated areas from sun exposure during healing to prevent complications and optimize results.
Preventing New Pre-Cancerous Lesions
If you’ve developed actinic keratoses or other pre-cancerous lesions, your skin has accumulated significant sun damage, and you’re at risk of developing more. Prevention becomes essential for protecting your skin health going forward.
Practice rigorous sun protection every day. Apply broad-spectrum sunscreen with SPF 30 or higher to all exposed skin, and reapply every two hours when outdoors. Wear protective clothing, including wide-brimmed hats, long sleeves, and sunglasses. Seek shade whenever possible, especially during peak UV hours between 10 a.m. and 4 p.m. Avoid tanning beds entirely.
Schedule regular skin examinations with Dr. Daoud. Because you’re at increased risk for developing additional pre-cancerous lesions and skin cancer, ongoing monitoring is important. The frequency of your examinations will depend on your individual risk factors and history.
Perform monthly self-examinations at home, checking for new or changing spots that should be evaluated.
Schedule Your Appointment Today
Pre-cancerous lesions are warning signs that shouldn’t be ignored. With prompt, appropriate treatment, you can eliminate these abnormal growths before they have a chance to become cancer. Dr. Shaza Daoud and the team at Glo Dermatology are here to provide the expert care you need to protect your skin health.
If you’ve noticed rough, scaly patches on sun-exposed skin, or if you’ve been previously diagnosed with actinic keratoses or other pre-cancerous conditions, contact our Parma office today at (216) 351-7700 to schedule your appointment. We welcome patients from throughout Greater Cleveland and Northeast Ohio, including Parma Heights, Brooklyn, Seven Hills, Independence, Middleburg Heights, and surrounding communities.
Take action now—treating pre-cancerous lesions is one of the most effective ways to prevent skin cancer.
Frequently Asked Questions About Pre-Cancerous Lesions
Are pre-cancerous lesions the same as skin cancer?
No. Pre-cancerous lesions are abnormal growths that have the potential to become cancer but haven’t yet. They represent an early stage in the development of skin cancer and can be treated before cancer develops. However, if left untreated, some pre-cancerous lesions will progress to skin cancer.
How can I tell if a spot is pre-cancerous?
Pre-cancerous lesions like actinic keratoses often feel rough or scaly, like sandpaper, even before they’re clearly visible. They typically appear on sun-exposed areas and may be red, pink, tan, or skin-colored. However, many skin conditions can look similar, so professional evaluation is the only reliable way to diagnose pre-cancerous lesions.
Do all actinic keratoses become cancer?
No. Most actinic keratoses don’t progress to cancer. However, an estimated 5 to 10 percent will become squamous cell carcinoma if left untreated. Since there’s no way to predict which lesions will progress, treatment of all actinic keratoses is recommended.
Is treatment painful?
Most treatments cause some discomfort, but pain is generally manageable. Cryotherapy causes a brief stinging or burning sensation. Topical treatments cause skin irritation during the treatment period. Dr. Daoud can discuss pain management options and help you choose a treatment approach you’re comfortable with.
Will pre-cancerous lesions come back after treatment?
Individual treated lesions shouldn’t return if fully destroyed. However, if you have sun-damaged skin, you may develop new pre-cancerous lesions in other areas over time. This is why ongoing sun protection and regular skin examinations are so important.
How can I prevent pre-cancerous lesions?
Protecting your skin from ultraviolet radiation is the key to prevention. Use sunscreen daily, wear protective clothing, seek shade, and avoid tanning beds. While you can’t undo past sun damage, you can prevent further damage and reduce your risk of developing additional lesions.
