Fungal Infection Treatment in Parma, Ohio
Fungal infections of the skin, hair, and nails are among the most common conditions dermatologists treat. If you’re dealing with the persistent itch of athlete’s foot, the embarrassment of toenail fungus, or the frustration of a ringworm infection that won’t clear up, you’re not alone—and effective treatment is available. At Glo Dermatology in Parma, Ohio, Dr. Shaza Daoud provides expert diagnosis and treatment for all types of fungal infections, helping patients throughout Greater Cleveland find relief and restore healthy skin and nails.
Fungal infections can be stubborn, often requiring targeted treatment and patience to fully resolve. Over-the-counter remedies work for some mild infections, but many fungal conditions need prescription-strength medications to clear completely. Dr. Daoud will accurately identify the type of fungal infection you’re experiencing and develop a personalized treatment plan to eliminate it and prevent recurrence. At Glo Dermatology, we combine medical expertise with compassionate care to help you overcome these common but bothersome conditions.
Understanding Fungal Infections
Fungi are microscopic organisms that exist all around us—in the air, soil, water, and on plants and surfaces. Many types of fungi are harmless, and some are even beneficial. However, certain fungi can cause infections when they come into contact with human skin, hair, or nails and find conditions favorable for growth.
Fungal infections thrive in warm, moist environments. This is why they commonly affect areas of the body that are warm and damp, such as the feet, groin, and skin folds. Fungi can spread through direct contact with an infected person or animal, contact with contaminated surfaces (like locker room floors or shared towels), or contact with infected soil.
While fungal infections are rarely dangerous in healthy individuals, they can cause significant discomfort, embarrassment, and frustration. Without proper treatment, fungal infections often persist indefinitely and may spread to other parts of the body or to other people. Certain populations, including people with diabetes, weakened immune systems, or circulatory problems, may be at higher risk for complications from fungal infections.
Types of Fungal Infections We Treat
Glo Dermatology treats all types of fungal infections affecting the skin, hair, and nails. Below are the most common fungal conditions we see in our Parma practice.
Athlete’s Foot (Tinea Pedis)
Athlete’s foot is one of the most common fungal infections, affecting up to 25 percent of the population at any given time. Despite its name, you don’t have to be an athlete to develop this condition—anyone can get it. Athlete’s foot typically causes itching, burning, and stinging between the toes or on the soles of the feet. The skin may appear red, scaly, dry, or cracked. In some cases, blisters may form. Without treatment, athlete’s foot can spread to the toenails and other parts of the body.
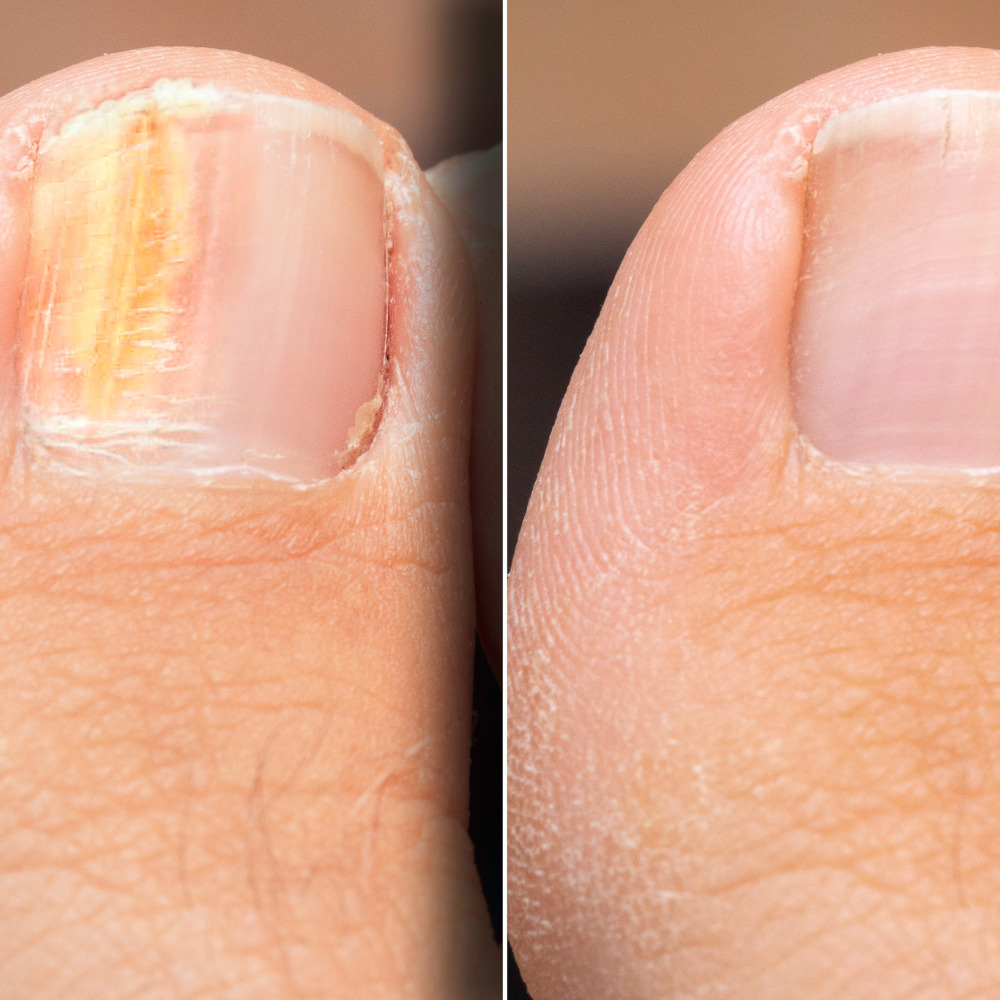
Toenail Fungus (Onychomycosis)
Fungal nail infections cause nails to become thickened, discolored, brittle, and crumbly. The condition typically begins as a white or yellow spot under the tip of the nail and gradually spreads deeper into the nail. Toenails are affected more often than fingernails because feet spend more time in the warm, moist environment inside shoes. Nail fungus is notoriously difficult to treat and often requires months of therapy to fully resolve.
Ringworm (Tinea Corporis)
Despite its name, ringworm is not caused by a worm—it’s a fungal infection that gets its name from the characteristic ring-shaped rash it produces. Ringworm of the body appears as circular, red, scaly patches with raised borders and clearer centers. The patches may be itchy and can occur anywhere on the body. Ringworm is highly contagious and can spread through direct contact with infected people, animals, or contaminated objects.
Jock Itch (Tinea Cruris)
Jock itch is a fungal infection affecting the groin, inner thighs, and buttocks. It causes a red, itchy, often ring-shaped rash in these warm, moist areas. Jock itch is more common in men and adolescent boys but can affect anyone. It often occurs in people who sweat heavily or who wear tight-fitting underwear or athletic supporters.
Scalp Ringworm (Tinea Capitis)
Scalp ringworm primarily affects children, though adults can develop it too. This infection causes scaly, itchy patches on the scalp that may be accompanied by hair loss in the affected areas. The patches may appear as black dots where hair has broken off at the scalp. Scalp ringworm is highly contagious and often spreads among children in schools and daycare settings.
Yeast Infections (Candidiasis)
Candida is a type of yeast that normally lives on the skin and in the body without causing problems. However, when conditions allow it to overgrow, it can cause infections. Cutaneous candidiasis typically occurs in warm, moist skin folds such as the armpits, groin, under the breasts, and between fingers or toes. It causes red, itchy rashes that may have satellite lesions (smaller spots around the main rash). Oral thrush and other mucosal yeast infections are also caused by Candida overgrowth.
Tinea Versicolor (Pityriasis Versicolor)
Tinea versicolor is caused by a yeast that naturally lives on the skin. When it overgrows, it causes patches of skin that are lighter or darker than surrounding areas. These patches are most noticeable after sun exposure, when the affected skin doesn’t tan like normal skin. Tinea versicolor commonly appears on the chest, back, and upper arms. While not harmful, many people seek treatment for cosmetic reasons.
Risk Factors for Fungal Infections
While anyone can develop a fungal infection, certain factors increase your risk. Understanding these risk factors can help you take preventive measures and recognize when you may be more susceptible.
Warm, moist environments create ideal conditions for fungal growth. People who sweat heavily, wear tight or non-breathable clothing and footwear, or spend time in humid environments are more prone to fungal infections. Shared facilities like locker rooms, swimming pools, and communal showers are common sources of exposure.
Certain health conditions increase susceptibility to fungal infections. Diabetes affects circulation and immune function, making infections more likely and harder to treat. Weakened immune systems, whether from illness, medication, or other factors, reduce the body’s ability to fight off fungal invaders. Poor circulation, obesity, and conditions that cause skin folds also increase risk.
Age plays a role as well. Nail fungus becomes increasingly common with age due to slower nail growth, reduced circulation, and years of exposure. Children are more susceptible to scalp ringworm, likely due to close contact with other children and developing immune systems.
Lifestyle factors matter too. Athletes and people who exercise frequently are more prone to athlete’s foot and jock itch due to sweating and use of shared facilities. Walking barefoot in public areas increases exposure to fungi. Wearing artificial nails or nail polish for extended periods can trap moisture and promote nail fungus.
Diagnosing Fungal Infections
Accurate diagnosis is essential for effective fungal infection treatment. While many fungal infections have characteristic appearances, other skin conditions can look similar, and using the wrong treatment can delay healing or worsen the problem.
During your appointment at Glo Dermatology, Dr. Daoud will examine the affected area and ask about your symptoms, when they started, and any treatments you’ve already tried. In many cases, the appearance and location of the infection provide enough information for diagnosis.
When confirmation is needed, Dr. Daoud may perform additional testing. A KOH (potassium hydroxide) preparation involves scraping a small sample of skin, nail, or hair and examining it under a microscope after treatment with KOH solution, which dissolves skin cells and makes fungal elements easier to see. Fungal cultures involve growing the organism in a laboratory to identify the specific type of fungus, which can help guide treatment selection. Wood’s lamp examination uses ultraviolet light to detect certain fungal infections that fluoresce under this light.
These diagnostic tools help ensure you receive the correct diagnosis and most effective treatment for your specific infection.
Fungal Infection Treatment Options
Treatment for fungal infections depends on the type of infection, its location and severity, and your overall health. Dr. Daoud will recommend the most appropriate treatment approach for your specific situation.
Topical Antifungal Medications
For many skin fungal infections, topical antifungal medications are the first-line treatment. These creams, ointments, powders, or sprays are applied directly to the affected area. Common topical antifungals include clotrimazole, miconazole, terbinafine, and ketoconazole. Over-the-counter formulations are available for mild infections, while prescription-strength versions provide more powerful treatment for stubborn cases. Treatment duration varies but typically ranges from two to four weeks for skin infections.
Oral Antifungal Medications
Some fungal infections require oral antifungal medications that work from the inside. Nail fungus almost always requires oral treatment because topical medications have difficulty penetrating the nail to reach the infection. Scalp ringworm also requires oral therapy because the fungus infects hair follicles beneath the skin surface. Severe or widespread skin infections may respond better to oral treatment as well. Common oral antifungals include terbinafine, itraconazole, and fluconazole. Treatment duration varies from several weeks for skin infections to several months for nail fungus.
Medicated Nail Lacquers
For mild to moderate nail fungus, medicated nail lacquers may be prescribed alone or in combination with oral medications. These antifungal polishes are applied to the affected nails daily or weekly, depending on the product. While less effective than oral medications for severe infections, nail lacquers can be a good option for patients who cannot take oral antifungals or prefer to avoid them.
Laser Treatment for Nail Fungus
Laser therapy for nail fungus uses focused light energy to kill fungal organisms within the nail. While research on effectiveness is ongoing, some patients find laser treatment helpful, particularly in combination with other therapies. Dr. Daoud can discuss whether laser treatment might be appropriate for your nail fungus.
Antifungal Shampoos
For scalp ringworm and tinea versicolor, medicated shampoos containing antifungal ingredients like ketoconazole or selenium sulfide may be recommended. These shampoos help reduce fungal organisms on the skin and scalp and are often used in combination with other treatments.
Treating Stubborn Nail Fungus
Toenail fungus deserves special mention because it is one of the most challenging fungal infections to treat. The nail plate acts as a barrier that prevents topical medications from reaching the infection, and fungi can persist in the nail bed even after the visible nail appears to improve.
Successful treatment of nail fungus requires patience and persistence. Oral antifungal medications are typically the most effective option, with treatment courses lasting three to six months or longer. Even with successful treatment, the nail takes time to grow out and appear normal—it can take a year or more for a toenail to fully replace itself.
During treatment, Dr. Daoud may recommend debridement (trimming and thinning the affected nail) to reduce the fungal load and improve medication penetration. Keeping nails clean and dry, wearing breathable footwear, and using antifungal powder in shoes can support treatment success.
Even after successful treatment, nail fungus has a tendency to recur. Ongoing preventive measures are important for maintaining healthy nails long-term.
Preventing Fungal Infections
Prevention is always preferable to treatment. While it’s not possible to avoid all fungal exposure, certain precautions can significantly reduce your risk of developing fungal infections.
Keep your skin clean and dry, especially in areas prone to moisture accumulation. Dry thoroughly between toes after bathing or swimming. Change out of sweaty clothes and damp swimsuits promptly. Use powder in areas where skin folds trap moisture.
Wear breathable footwear and moisture-wicking socks. Alternate shoes to allow them to dry completely between wearings. Replace athletic shoes regularly. Avoid tight, non-breathable shoes, especially in hot weather.
Protect your feet in public areas. Wear shower shoes or flip-flops in locker rooms, public showers, and around swimming pools. Never share shoes, socks, towels, or personal care items with others.
Care for your nails properly. Keep nails trimmed and clean. Avoid cutting cuticles, which protect against infection. If you get manicures or pedicures, choose salons that properly sterilize their instruments or bring your own tools.
Avoid contact with infected people, animals, or objects. If someone in your household has a fungal infection, take precautions to prevent spread, and ensure they receive proper treatment.
If you have diabetes or other conditions that increase infection risk, work with your healthcare providers to manage your condition and monitor for early signs of infection.
When to See a Dermatologist for Fungal Infections
While mild fungal infections may respond to over-the-counter treatments, you should see Dr. Daoud if your infection doesn’t improve after two weeks of self-treatment, the infection is severe, widespread, or affecting your nails, you have diabetes, a weakened immune system, or other health conditions that increase infection risk, you’re unsure whether your skin problem is actually a fungal infection, the infection keeps coming back despite treatment, or you’re experiencing significant discomfort or embarrassment.
Professional evaluation ensures accurate diagnosis and access to prescription-strength treatments that can resolve stubborn infections more effectively than over-the-counter options.
Schedule Your Fungal Infection Consultation Today
Fungal infections are common, treatable conditions—there’s no need to suffer with itching, discomfort, or unsightly nails. Dr. Shaza Daoud and the team at Glo Dermatology are here to help you identify and eliminate your fungal infection so you can enjoy healthy, comfortable skin and nails once again.
Take the first step toward relief by scheduling a consultation at our Parma office. Contact us today at (216) 351-7700 to book your appointment. We welcome patients from throughout Greater Cleveland and Northeast Ohio, including Parma Heights, Brooklyn, Seven Hills, Independence, Middleburg Heights, and surrounding communities.
Frequently Asked Questions About Fungal Infections
Are fungal infections contagious?
Yes, most fungal infections can spread from person to person through direct contact or through contact with contaminated surfaces, clothing, or personal items. Some fungal infections, like ringworm, can also spread from animals to humans. Taking precautions to avoid sharing personal items and maintaining good hygiene can help prevent transmission.
Why does my fungal infection keep coming back?
Recurrent fungal infections are common and can occur for several reasons. The original infection may not have been completely eliminated; reinfection may occur from contaminated shoes, socks, or environments, or conditions that favor fungal growth (moisture, warmth, tight clothing) may persist. Dr. Daoud can help identify why your infections recur and develop a comprehensive prevention strategy.
How long does it take to cure a fungal infection?
Treatment duration varies depending on the type and severity of the infection. Mild skin infections may clear in two to four weeks with topical treatment. Nail fungus typically requires three to six months of oral medication, and it can take a year or longer for the nail to grow out completely and look normal. Dr. Daoud will provide specific expectations based on your condition.
Can I treat nail fungus with home remedies?
While various home remedies (like tea tree oil, vinegar, or Vicks VapoRub) are popularly suggested for nail fungus, scientific evidence supporting their effectiveness is limited. These remedies may help mild cases but are unlikely to cure established infections. Prescription antifungal medications remain the most effective treatment for nail fungus.
Is athlete’s foot the same as toenail fungus?
Athlete’s foot and toenail fungus are both fungal infections often caused by the same organisms, but they affect different structures. Athlete’s foot affects the skin of the feet, while toenail fungus affects the nails. However, the two conditions are related—untreated athlete’s foot can spread to the toenails, and infected nails can serve as a reservoir for reinfecting the skin.
Can fungal infections spread to other parts of my body?
Yes, fungal infections can spread from one area of the body to another. For example, scratching athlete’s foot and then touching other areas can transfer the fungus to the groin (causing jock itch) or elsewhere on the body (causing ringworm). Good hygiene and prompt treatment help prevent this spread.
